Guidelines to Groceries: A U.S. Food Reset
The Dirt
The new USDA/HHS dietary guidelines marks a “historic reset” in U.S. nutrition policy with a straightforward message: eat real food. But how does this differ from current guidelines?
Nutrition
Guidelines to Groceries: A U.S. Food Reset
The Dirt
The new USDA/HHS dietary guidelines marks a “historic reset” in U.S. nutrition policy with a straightforward message: eat real food. But how does this differ from current guidelines?
Click Play to listen to our generated podcast. Access our full podcast library here.
This nutrition reset might sound simple, but the implications aren’t. Because federal dietary guidance doesn’t just shape dinner-table choices. It influences nutrition education, procurement standards, labeling conversations, school meals, and the broader public narrative around what counts as “healthy.”
And in the U.S., that narrative inevitably touches agriculture: what we grow, how we raise it, how we process it, and what ends up being affordable and accessible for families.
So what actually changed in these guidelines — and what should consumers and food-system stakeholders expect to come next?
What the New Guidelines Emphasize
The January 7, 2026 rollout frames the 2025–2030 Dietary Guidelines (DGA) as a “reset” toward real food and away from dietary advice that feels abstract, overly clinical, or too easy to game with marketing.
The easiest way to understand this “reset” is as a shift in what anchors a meal.
Previously, carbs were the base, with fat used cautiously. Now, meals are framed around protein, healthy fats, and whole produce. For dairy, guidance previously directed consumers to low-fat options, but now full-fat dairy is explicitly endorsed, as long as the food items don’t have added sugar. With a new focus on whole grains as part of a diet, guidance on consuming refined carbohydrates has now lowered, as well as limiting highly processed foods, added sugars, and artificial additives.

This isn’t just a new list of “eat more, eat less.” It’s a new public framing: less nutrition-by-math, more nutrition-by-common-sense.
Key Guideline Changes
‘You are what you eat’ has never been more evident. 60% of chronic diseases can be attributed to inflammatory diets. The press release argues the shift is necessary because of these rampant chronic disease trends, pointing to:
- Nearly 90% of U.S. health care spending going toward treating chronic disease
- More than 70% of American adults being overweight or obese
- Nearly 1 in 3 adolescents having prediabetes
Whether you agree with every policy implication or not, the framing is unmistakable: diet-related disease is positioned as a national readiness and economic issue, not just a personal-health issue.
Protein: Eat More at Every Meal
The guidelines urge Americans to “prioritize protein at every meal,” and the new document includes protein targets in the range of 1.2-1.6 g/kg/day, or about 0.5 grams of protein per pound of body weight per day.
Why this is being emphasized:
- Muscle maintenance: There’s growing attention to preserving lean mass across adulthood and aging, and protein plays a critical role in that.
- Satiety + weight management: Higher-protein patterns can help with fullness and sometimes weight-loss adherence (people naturally eat fewer calories when they feel satisfied by a food).
- A cultural reality: Protein has become the “macro Americans can understand,” which makes it an easy public message to repeat.
Was this driven by “new research”?
- Not in the simple way headlines suggest. There is a body of research looking at higher-protein approaches in certain contexts, but many experts argue most Americans already get adequate protein and that these higher targets may not be warranted for the general population. That critique is showing up immediately in mainstream reporting about the new guidelines.
Full-fat Dairy: Part of Healthy Diet
The guidelines explicitly recommend full-fat dairy with no added sugars.
Why this is being emphasized:
- Nutrient density + satiety: Dairy delivers protein, calcium, phosphorus, magnesium, and vitamins A,D,E, and K. The full-fat options tend to be more satisfying for many people. This also slows down the digestion of any milk sugars.
- A pushback against “low-fat but more sugar”: For years, many “low-fat” flavored dairy products compensated with sugar. The new framing tries to make “unsweetened” the non-negotiable.
Was this driven by “new research”?
- The evidence around dairy fat and health outcomes has been clear at least since 2002, but the ‘low fat’ diet from the 1950s prevailed. The saturated fat in whole dairy was blamed for cardiovascular disease and weight gain, but research shows this is not the case.
- Saturated fat guidance has been a consistent feature of prior DGAs and remains a major topic in the DGA report.
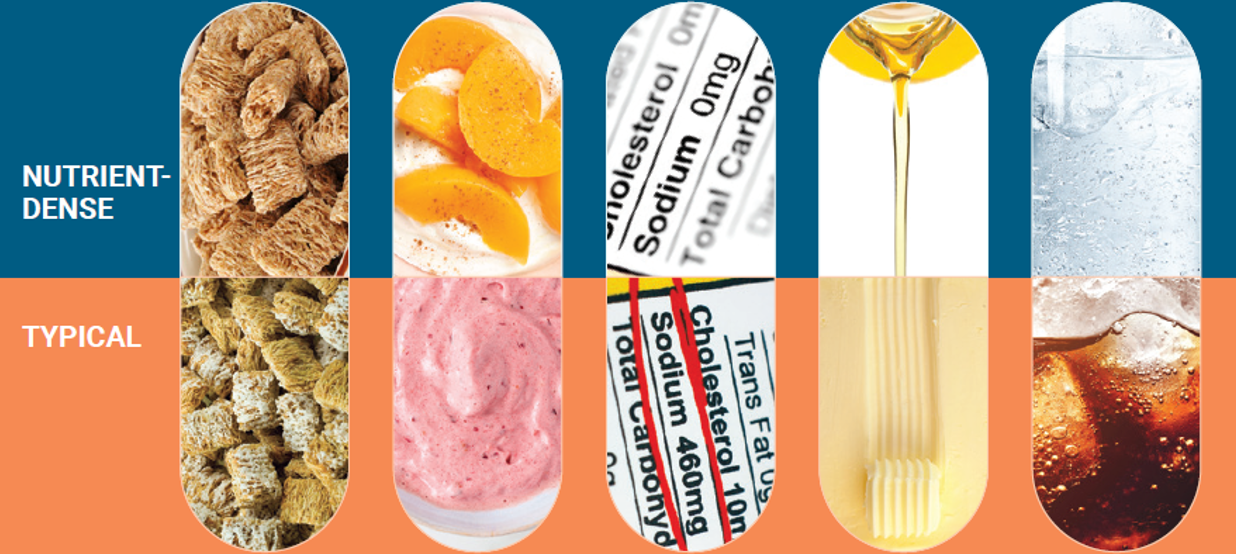
Produce: Eat Whole Fruits & Veggies All Day
The guidelines stress eating vegetables and fruit throughout the day, focusing on whole forms.
Why this is being emphasized:
- This is the least controversial part of the reset. The U.S. has long-standing shortfalls in fruit/vegetable intake, and whole forms generally deliver fiber and better satiety than juice or heavily sweetened “fruit products.”
Was this driven by new research?
- Not “new,” so much as overwhelming continuity: long-term evidence consistently supports produce-rich dietary patterns for cardiometabolic health.
- Eat the rainbow is an easy way to remember to get your 5-7 servings of fruit and vegetable in a day.
Healthy Fats: Consume from Whole Foods & Meats
The guidelines state to incorporate healthy fats from whole foods such as meats, seafood, eggs, nuts, seeds, olives, and avocados.
Why this is being emphasized:
- The growing body of research, supporting the importance of the omega 3’s and 6’s for brain health and anti-inflammatory benefits
- Lower-carb messaging needs a replacement calorie source: If you reduce refined carbs and added sugar, you inevitably talk about what replaces them. “Healthy fats” fills that gap.
- Less fear-based fat messaging: It reflects a broader public shift away from blanket “fat is bad” thinking.
Was this driven by new research?
- This is more of an interpretive evolution than a single new study.
- The strongest consensus has long been around types of fat and overall dietary patterns, rather than fat avoidance at all costs, but where specific foods land is still debated.
Whole Grains: Ok to Eat, Reduce Refined Carbs
The guidelines suggest that we focus on whole grains while sharply reducing refined carbohydrates.
Why this is being emphasized:
- Refined carbs are an easy “common enemy” because they’re overconsumed, highly palatable, and often bundled with added sugars and sodium in packaged foods.
- Shifting people toward whole grains typically increases fiber and micronutrients without demanding perfection.
Was this driven by new research?
- It’s consistent with decades of diet-quality research and the reality of current U.S. intake patterns (too many refined grains, too few whole grains).
Limit Highly Processed Foods
The new guidelines urge us to limit ultra-processed foods, added sugars, and artificial additives.
Why this is being emphasized:
- This reflects a major cultural and scientific focus over the last decade: ultra-processed dietary patterns are associated with poorer health outcomes in many observational studies, and controlled feeding studies are exploring mechanisms and causality.
Was this driven by new research?
- There has been a surge in research of ultra-processed foods (UPF) that these products may negatively affect our health.
- While there is no use of the term “UPF” in the guidelines, they do note that older adults may need “fortified foods or supplements” under medical supervision if their “dietary intake or absorption is insufficient.”
Can We Reset in The Real World?
And this is the tension consumers live in every day.

The foods most people recognize as healthy are often the foods that feel hardest to execute consistently because of cost, time, cooking skills, kitchen access, and family preferences.
The Dietary Guidelines can call for a “real food” reset, but the how matters just as much as the what. To their credit, HHS messaging tries to preempt the practicality critique by emphasizing flexibility—fresh, frozen, dried, or canned all count.
But if federal guidance is going to land with everyday households, it has to translate into real-world realities like:
- What “protein at every meal” looks like in school cafeterias, quick-service restaurants, and tight grocery budgets
- How “limit ultra-processed foods” intersects with the fact that processed foods are often the most shelf-stable, accessible options
- How emerging research (like the more nuanced conversation around full-fat dairy) actually makes its way into schools, doctor’s offices, and public health messaging—especially while debates around saturated fat and population-level guidance remain unresolved in global forums
Even if you never read the full document, the consumer takeaways are familiar—and workable when you frame them as practical defaults, not perfection:
- Build meals around a protein anchor (eggs, yogurt, beans, fish, poultry, lean beef, tofu)
- Add produce in the form you’ll actually use (fresh or frozen)
- Choose whole grains more often and cut back on refined carbs and added sugars
- Be skeptical of health halos; prioritize foods that are straightforward, filling, and nutritionally complete
- The 2025–2030 Guidelines are being positioned as a major reset with a clear theme: real food, more protein, whole fruits and vegetables, healthy fats, whole grains, and fewer ultra-processed foods and added sugars. But implementation—what people can afford, access, and realistically repeat—is where this “reset” will either succeed or stay stuck on paper.
What This Mean for Ag & Food Producers
This is where D2D readers should pay close attention: when federal guidance elevates specific categories (protein, dairy, produce, whole grains), it tends to reinforce demand signals across supply chains.
Potential downstream effects to watch:
- Protein demand stays front-and-center
The guidelines explicitly spotlight protein “at every meal,” which supports ongoing momentum for animal and plant protein production, and innovation in how protein is packaged, priced, and distributed. - Dairy — especially full-fat — gets a reputational lift
The recommendation for “full-fat dairy with no added sugars” is a direct reversal of the cultural push many consumers grew up with. And it aligns with the Whole Milk for Healthy Kids Act, signed January 14, 2026, bringing whole milk back into school meals, a concrete example of how guidance can translate into policy and purchasing. - A renewed premium on minimally processed “value-added” foods
The line between “processed,” “ultra-processed,” and “convenient but still nutritious” is where brands will compete. The winners may be foods that do the hard work for consumers, while keeping ingredient lists simple and benefits clear.
The Bottom Line
For consumers, this is a simplified North Star. For agriculture and food producers, it’s a strong signal about where federal nutrition messaging — and potentially purchasing and policy — may head next. The real test won’t be the press release. It will be whether this guidance can translate into affordable, accessible, realistic eating patterns for American families.